
Our eyesight is a precious function that many of us take for granted. While sitting in the doctor’s office may not be something you enjoy doing, a yearly visit with your ophthalmologist is a great way to protect your vision from degenerative eye disease. Supplements and vitamins are used for slowing or stopping the progression of macular degeneration in older adults. Macular degeneration is the most common eye disease. If you are 55 years or older, your ophthalmologist should examine your eyes every year as early diagnosis is the key to a successful treatment plan.
What Causes Macular Degeneration?
There are many risk factors for macular degeneration such as heredity and age, smoking, high blood pressure, and vitamin-deficient diets.
The two types of macular degeneration are wet and dry. Both will lead to loss of vision if they are not diagnosed and treated aggressively. For more information on risk levels and the types of macular degeneration, contact your ophthalmologist.
If you have been diagnosed with macular degeneration, you are not alone. While macular degeneration is a leading cause of blindness, it is also treatable. Depending on your level of degeneration and your adherence to a treatment plan, you can slow the development of macular degeneration for many years.
Supplements for Macular Degeneration
There are many treatments available for macular degeneration patients, and your specific treatment options will depend on the type, stage, and personal medical history.
Remember, your ophthalmologist is a trained professional, so regardless of the treatment recommended, following it closely is imperative to maintaining your vision. The first step to stopping or slowing the spread of macular degeneration is adjusting your diet to include supplements to improve your health. Here is a list of the most common changes for your diet:
1. Zinc and Antioxidants
After years of research, studies have shown that taking supplements with high levels of zinc and antioxidants may help slow the progression of macular degeneration. Your ophthalmologist will recommend the right type and dosage of these supplements. If you are at risk of developing macular degeneration or are concerned about this condition, ensure your daily multivitamin contains these vital nutrients.
Tips & Insights: Should I Get Cataract Surgery? Benefits & Suggestions
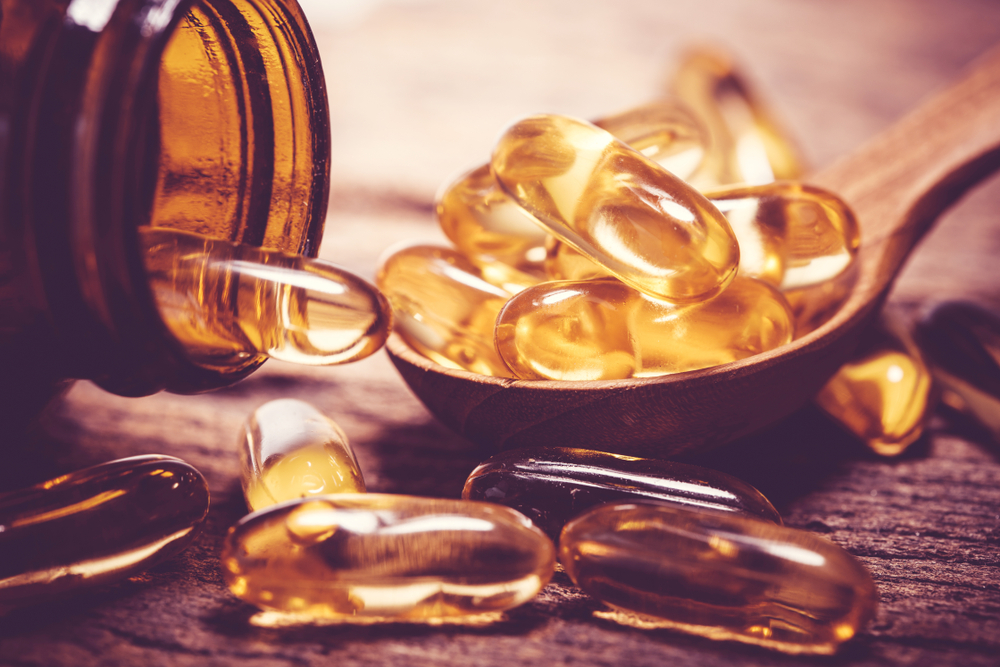
2. Other Vitamins and Minerals
In addition to zinc and antioxidants, the American Academy of Ophthalmology recommends a daily supplement with high doses of vitamins C and E, copper, and zeaxanthin. This regimen is based on recent findings that suggest these supplements may stop or slow the progression of intermediate dry macular degeneration from advancing to wet macular degeneration, the stage when loss of vision occurs.
3. Eye-Healthy Foods
While supplements are the most common treatment for macular degeneration, remember that simply taking a daily vitamin will not prevent or slow the progression of this destructive disease.
Ophthalmologists also recommend, in addition to daily supplements, eating a diet rich in nutrients that promote healthy eye function and slow the advancement of macular degeneration. When choosing fruits and vegetables, choose colorful vegetables, particularly dark leafy greens like spinach and kale.
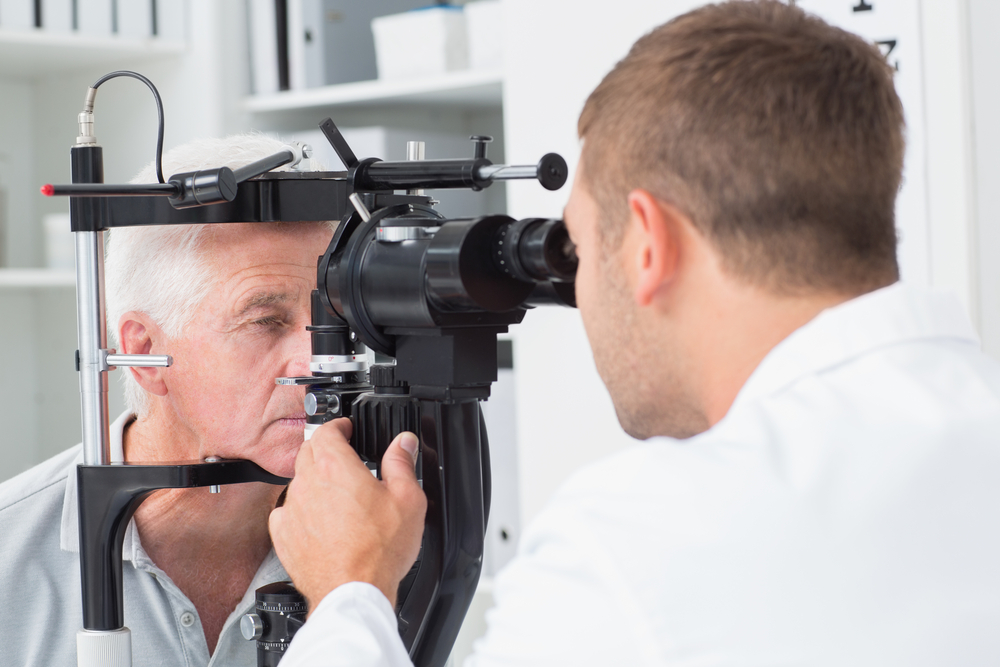
Preventing Macular Degeneration
Your best defense against developing a degenerative eye disease is to practice preventative measures, so macular degeneration will not be a threat to your eyesight. Regular eye exams and tools like the Amsler Grid test can help detect any changes in the retina and macula. Our staff of ophthalmologists provides dependable eye care solutions such as macular degeneration treatments, cataract surgery, dry eye treatments, LASIK eye surgery, and presbyopia treatments. Yearly examinations with our team of ophthalmologists will verify that your eyes are healthy. If they're not, yearly exams allow for early detection of eye degeneration.
We'll help you to utilize the many treatments, supplements, and vitamins for macular degeneration if this condition affects you. Our team of ophthalmologists offers eye treatment options in areas of Michigan and Ohio such as Ann Arbor, Kalamazoo, Bryan, and Toledo. Schedule an appointment online or call us at (877) 852-8463.
 877-852-8463
877-852-8463 Careers
Careers Locations
Locations Patient Portal
Patient Portal Request Appointment
Request Appointment







 877-852-8463
877-852-8463
